Cirrhosis of the liver is a serious, progressive condition that develops over time as the liver sustains repeated injury. Unlike sudden illnesses, cirrhosis does not appear overnight—it evolves through distinct stages of liver disease, often silently, before severe symptoms appear. Understanding these stages is critical for early detection, prevention, and management.
The liver is one of the most resilient organs in the human body. It performs more than 500 essential functions, including detoxifying harmful substances, producing bile for digestion, regulating blood clotting, and storing vital nutrients. However, when the liver is repeatedly damaged—due to infections, alcohol use, metabolic disorders, or chronic inflammation—it begins to scar. Over time, this scarring disrupts normal liver function and can ultimately lead to liver failure.
Contact Us

In this article, we’ll explore the four stages of cirrhosis of the liver, how they progress, common causes, symptoms to watch for, and why early intervention can be life-saving.
Overview: The 4 Stages of Liver Disease Leading to Cirrhosis
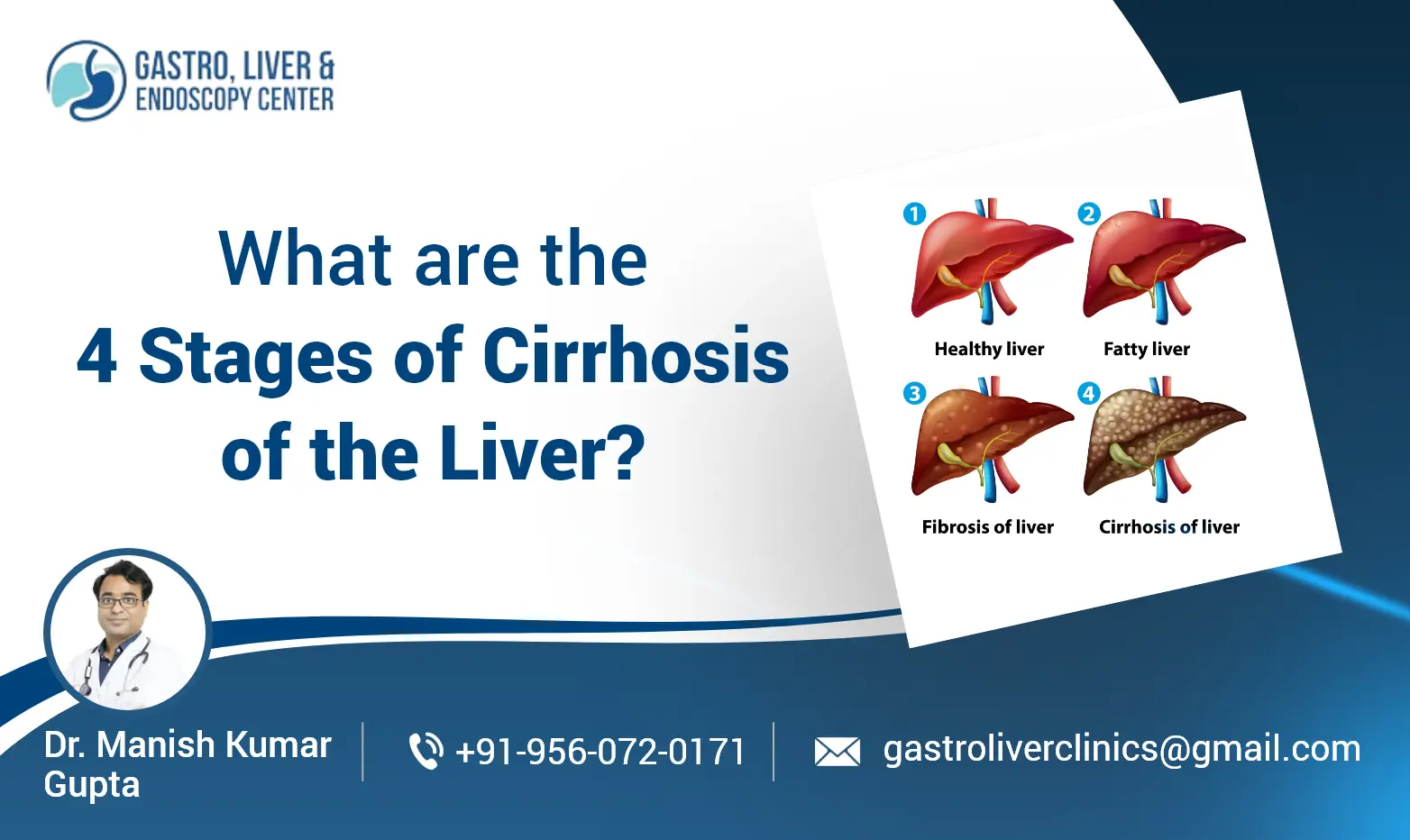
Liver disease generally progresses through the following stages:
- Hepatitis (Inflammation / Fatty Liver)
- Fibrosis (Scarring)
- Cirrhosis (Severe Scarring / Hardened Liver)
- Liver Failure (End-Stage Liver Disease)
Each stage represents increasing damage to liver tissue. Let’s break down each stage in detail.
Stage 1: Hepatitis (Inflammation / Fatty Liver Disease)
What Happens at This Stage?
The earliest stage of liver disease is hepatitis, which simply means inflammation of the liver. This inflammation may occur due to infections (such as hepatitis B or C), excessive alcohol intake, obesity, insulin resistance, or exposure to toxins and certain medications.
A common form of early liver disease is steatosis, also known as fatty liver disease. At this stage, fat accumulates inside liver cells, triggering inflammation. Importantly, liver cells are still largely intact, and the liver can continue functioning normally.
Common Causes
- Excessive alcohol consumption
- Non-alcoholic fatty liver disease (NAFLD)
- Viral hepatitis (A, B, C)
- Poor diet and obesity
- Diabetes and metabolic syndrome
- Certain medications or toxins
Symptoms
Most people experience no symptoms at this stage. When symptoms do occur, they may include:
- Fatigue
- Mild abdominal discomfort
- Feeling unwell or sluggish
- Slightly elevated liver enzymes on blood tests
Is It Reversible?
Yes. This stage is often completely reversible with lifestyle changes, treatment of the underlying cause, and medical monitoring. This makes early detection especially important.
Stage 2: Fibrosis (Scarring of the Liver)
What Happens at This Stage?
When inflammation persists over time, the liver attempts to repair itself. Unfortunately, this healing process leads to the formation of scar tissue (fibrosis). Scar tissue replaces healthy liver cells and begins to interfere with normal liver function and blood flow.
At this stage, the liver is still able to perform many of its essential tasks, but efficiency starts to decline.
What Fibrosis Means
Fibrosis is not yet cirrhosis, but it is a critical warning sign. The scarring is still limited, and some healthy liver tissue remains.
Symptoms
Symptoms are often mild or absent but may include:
- Ongoing fatigue
- Loss of appetite
- Mild swelling in the abdomen
- Elevated liver enzymes
Is It Reversible?
Fibrosis may be partially reversible, especially if the underlying cause is addressed early. Stopping alcohol use, managing viral hepatitis, losing weight, and controlling blood sugar can slow or even halt progression.
Stage 3: Cirrhosis (Severe Scarring and Liver Hardening)
What Happens at This Stage?
Cirrhosis occurs when scar tissue becomes widespread and permanent, replacing much of the healthy liver tissue. The liver becomes hardened, shrunken, and distorted, significantly impairing blood flow and liver function.
At this point, the damage is extensive, and the liver struggles to perform its essential roles.
Compensated vs. Decompensated Cirrhosis
- Compensated cirrhosis: The liver is damaged but still manages to function.
- Decompensated cirrhosis: Serious complications arise, indicating liver failure is approaching.
Symptoms
Symptoms become more noticeable and may include:
- Persistent fatigue and weakness
- Jaundice (yellowing of skin and eyes)
- Easy bruising or bleeding
- Swelling in legs and abdomen (edema and ascites)
- Itchy skin
- Digestive issues
Is It Reversible?
Cirrhosis is generally not reversible, but progression can often be slowed with treatment, lifestyle changes, and medical management. Early diagnosis at this stage can still significantly improve quality of life and survival.
Stage 4: Liver Failure (End-Stage Liver Disease)
What Happens at This Stage?
In the final stage, the liver is so severely damaged that it can no longer perform its vital functions. This condition is known as end-stage liver disease (ESLD) or hepatic failure.
Blood toxins are no longer filtered properly, fluid accumulates in the body, and the risk of life-threatening complications increases dramatically.
Common Complications
- Ascites (fluid buildup in the abdomen)
- Jaundice
- Hepatic encephalopathy (confusion, memory loss, personality changes)
- Variceal bleeding (ruptured veins in the esophagus or stomach)
- Kidney failure
- Infections
Symptoms
- Severe fatigue
- Confusion or altered mental state
- Severe swelling in abdomen and legs
- Dark urine and pale stools
- Shortness of breath
- Muscle wasting
Treatment Options
At this stage, treatment focuses on:
- Managing symptoms and complications
- Preventing infections
- Improving quality of life
For many patients, a liver transplant is the only definitive treatment.
Why Understanding the Stages Matters
Recognizing the stages of liver disease helps patients and healthcare providers:
- Detect liver damage early
- Prevent progression to cirrhosis
- Improve treatment outcomes
- Reduce complications and mortality
The earlier liver disease is diagnosed, the greater the chance of stopping or slowing its progression.
FAQs:
Q1. Can cirrhosis develop without symptoms?
A1. Yes. Many people have liver disease or even early cirrhosis without noticeable symptoms, which is why routine checkups are important.
Q2. How long does it take to progress through the stages?
A2. Progression varies widely. It may take years or decades, depending on the cause, lifestyle, and treatment.
Q3. Is fatty liver always dangerous?
A3. Fatty liver itself is often reversible, but if untreated, it can progress to fibrosis and cirrhosis.
Q4. Can cirrhosis be cured?
A4. Cirrhosis cannot usually be cured, but treatment can slow progression and manage symptoms. A liver transplant may offer a cure in advanced cases.
Q5. What are the most common causes of cirrhosis?
A5. Alcohol abuse, chronic viral hepatitis, non-alcoholic fatty liver disease, and autoimmune liver diseases are leading causes.
Q6. Can you live a normal life with cirrhosis?
A6. Many people with compensated cirrhosis live for years with proper medical care and lifestyle changes.
Q7. How is cirrhosis diagnosed?
A7. Diagnosis may include blood tests, imaging studies, elastography, and sometimes a liver biopsy.
Q8. Does cirrhosis always lead to liver failure?
A8. Not always. Early detection and treatment can prevent or delay progression to liver failure.
Q9. What lifestyle changes help protect the liver?
A9. Avoid alcohol, maintain a healthy weight, eat a balanced diet, exercise regularly, and manage chronic conditions like diabetes.
Q10. When is a liver transplant needed?
A10. A transplant is considered when the liver can no longer function adequately and complications cannot be controlled with medical treatment.
Final Thoughts
Cirrhosis is the result of long-term liver damage, but it doesn’t happen all at once. Understanding the four stages of cirrhosis of the liver—from early inflammation to end-stage liver failure—empowers individuals to take action early. With timely diagnosis, proper medical care, and lifestyle changes, it is often possible to slow progression, reduce complications, and significantly improve quality of life.
If you suspect liver disease or have risk factors, consult a healthcare professional—your liver’s health matters more than you think.